On Diagnosis
This page is intended for people who have or are parents of a child who has recently been diagnosed with a PTEN gene alteration or who are awaiting the result of a genetic test.
If you have waited a very long time to get a diagnosis to account for multiple medical problems, it may come as something of a relief to find out that there is a reason behind these. For many people though, it is a difficult and daunting time.
What makes doctors think to test the PTEN gene?
Single gene testing
Genetic conditions often cause a pattern or “syndrome” of features. When doctors familiar with rare genetic conditions see particular health or developmental problems clustering together in a person or in a family, they may recognise that an alteration or “mutation” in a single gene is likely to be responsible for that pattern or “syndrome”. So, if a person has lots of issues often associated with alterations in the PTEN gene, a doctor might be fairly confident that the gene test will find an alteration in the gene. A family history of certain health and developmental problems will increase the suspicion that an alteration in the PTEN gene will be found.
If a person has only a few features (for example in a young child) associated with variation in the PTEN gene, the doctor will be less certain that the gene test will find a PTEN mutation, but they will have enough suspicion to order the test.
Will the genetic test always find a PTEN gene alteration if it is there?
Even when someone has lots of health problems or features of a PTEN gene alteration, a genetic test may not find a gene alteration. Your doctor will check that the test included looking for point mutations (like a spelling mistake in a word) and larger deletions (a part of the gene is missing). If the PTEN gene test doesn’t find the cause, the doctor might think about testing other genes. The doctor may ask you if you would like to participate in the 100,000 genomes project.
https://www.genomicsengland.co.uk/the-100000-genomes-project/
https://www.genomicsengland.co.uk/taking-part/
Panel testing
Increasingly, genes are tested as panels. Panel tests enable doctors to test many genes at once. A panel might include genes that cause cancers, or genes that cause developmental delay or intellectual difficulties. Testing lots of genes at once is quicker and cheaper than testing one gene at a time. They are generally used when someone has significant developmental or health problems, but when these don’t fit into a pattern specific enough for the doctor to consider requesting a single gene test.
How are genetic tests done? What does it involve?
A genetic test is usually done on a blood sample. It will take at least a few weeks and up to about 4 months for your doctor to get the result back.
- Learn about Genetics – https://www.geneticalliance.org.uk/information/learn-about-genetics/
- Genes and Chromosomes – https://www.geneticalliance.org.uk/information/learn-about-genetics/dna-genes-chromosomes-and-mutations/
- What is a genetic test? – https://www.geneticalliance.org.uk/information/services-and-testing/what-is-a-genetic-test/
My/my child’s symptoms fit with what is described here. How do I get a genetic test?
If you see a hospital doctor, they may be able to request genetic testing for you. You can ask to be referred to your closest genetics service.
https://www.geneticalliance.org.uk/information/services-and-testing/nhs-genetic-services-in-the-uk/
What are the symptoms that would make a doctor think to order a PTEN gene test?
In children
- A big head (macrocephaly) – usually at the top of the growth chart or even above the top line on the growth chart. The other growth measurements might be at or near the top of the chart too, but not always.
- Developmental delay – babies and young children may be late to achieve their motor milestones e.g. rolling, sitting, standing and walking. (In my experience, all children achieve these, but I don’t have data about by what age)
- Delayed speech and language – many children need speech and language therapy
- Autism or autistic features – some children with a PTEN gene alteration will be diagnosed with autism. This is a term that describes a pattern of behaviour. For most children with autism, the underlying cause is not found with current genetic tests. Alterations in the PTEN gene are a cause of autism but most people with an alteration in this gene are not autistic. Between 10% and 20% of children with a big head (macrocephaly) and autism have a gene alteration in the PTEN gene.
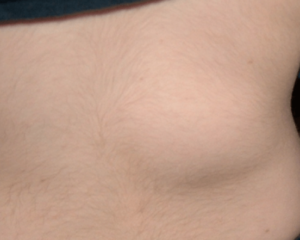
- Lipomas – these are soft lumps on the skin, filled with fat. They are harmless, unless they occur in places that cause irritation e.g on the foot where shoes rub or where a belt or other clothing straps rub.
- Malformations in blood vessels (vascular malformations) – these may be lumps or tangles of blood vessels under the skin (haemangiomas or arterio-venous malformations)
- Skin lumps and bumps – children may have skin features associated with PTEN gene alterations. People tend to develop more of these as they grow older and this means that making the diagnosis based on the skin features is often difficult or not possible in young children. (see adult section for more details).
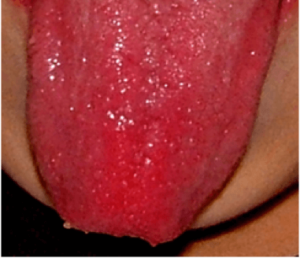
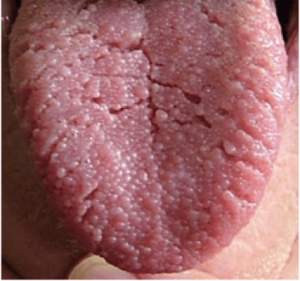
- Other features include lumpy gums and little growths inside the mouth (papilloma), freckling of the penis (under the foreskin – this can be difficult to examine in young boys as the foreskin does not draw back).
- Polyps in the bowel can occur too. The histology (how the polyp appears after removal when looking down a microscope) is variable, but benign (not cancerous). They are discovered when symptoms including chronic diarrhoea are investigated with a colonoscopy. Sometimes a single large polyp can cause these symptoms, which after removal of the polyp the symptoms are resolved. Sometimes symptoms are caused by multiple small polyps, which can be more difficult to treat.
What else might happen in childhood?
- Thyroid nodules might be identified. They can be picked up on an ultrasound scan of the neck. There are rare reports of thyroid cancer in childhood in the medical literature. It is so rare, that in the UK, it is not routine to screen children with a PTEN gene alteration for thyroid problems.
- Recent reports suggest that some children with a PTEN gene alteration have an abnormality of their immune system. There are limited reports about this so far. If a child is getting lots of infections, a doctor might request blood tests to examine the child’s immune system.
Why might a doctor request a PTEN gene test in an adult?
Often a diagnosis of a PTEN gene alteration is not made until well into adult life. The condition is very variable and some people with a PTEN gene alteration have no significant health or developmental problems in childhood, or in some cases, in adulthood. People diagnosed with a PTEN gene alteration in adulthood may, with hindsight, recognise that they did have symptoms in childhood. These may have been so mild that they did not get investigated. Other people will have had significant issues in childhood, but could not have got an earlier diagnosis as the gene was identified only in 1997 (Liaw et al, Arch et al). Some people may know they have a condition associated with PTEN gene alterations, but not actually had a genetic test.
What symptoms can occur for the first time in an adult with a PTEN gene alteration?
In addition to the symptoms described above in children
Cancer is a common disease; for example 1 in 8 women will develop breast cancer in their lifetime. What is unusual about people with a PTEN gene alteration (and people with alterations in other cancer predisposition genes) is that they are at risk of developing cancer earlier in life than is usual. As a general rule, this means cancer that affects someone before the age of 50.
People with PTEN can develop breast cancer, particular types of thyroid cancer, kidney cancer (renal cancer), cancer of the womb lining (endometrial cancer) and bowel cancer.
A rare condition, called Lhermitte-Duclos syndrome can occur in people with a PTEN gene alteration. It is a growth in the back part of the brain called the cerebellum. It is not a cancer, but as it grows it can cause increasing problems with symptoms such as blurry vision or increasing balance problems. If you have been diagnosed with Lhermitte-Duclos syndrome, testing of the PTEN gene may be considered, even if you don’t have other symptoms of PHTS.
A Clinical Geneticist will make recommendations for screening, based on guidelines agreed by the Cancer Genetics Group, a constituent group of the Clinical Genetics Society and British Society of Genomic Medicine.
Skin problems
People with an alteration in the PTEN gene can have skin features, which can help to point doctors towards the diagnosis. It is likely that only a Dermatologist or a Clinical Geneticist would recognise these. These are all benign (non-cancerous).
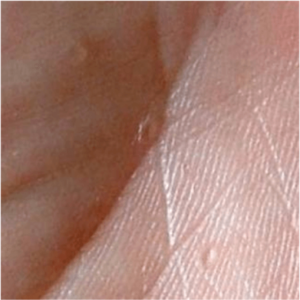
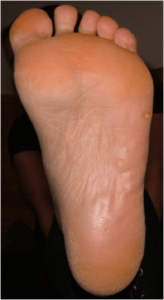
- Pitted keratoses are small pits on the palms of the hands or soles of the feet.
- Acral keratoses resemble verrucas.
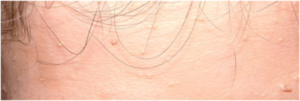
- Papillomatous papules are small, soft, skin coloured raised lumps.
- Trichilemmomas are small lumps arising on the face in a hair follicle.
Other lumps and bumps
Lumps and bumps can also occur on the moist lining of parts of the body, such as the mouth and digestive system.
Other health problems, which are not cancer are seen in people with PHTS. These include
- Thyroid nodules or cysts (lumps sometimes filled with fluid)
- Lumps and bumps in the breast tissue (fibrocystic disease) and growths in the womb called fibroids, can be particularly problematic in women with PHTS.
These problems are common health problems in people without a PTEN gene alteration. Testing of the PTEN gene would only be appropriate if these health problems were seen in combination with other health issues associated with PHTS.
Does everyone get all these problems?
No, people with a PTEN gene alteration may have some of these issues. It is rare for someone to have all of them. No-one currently knows the reason for the variability of the condition between people. The same is true of many other genetic conditions.
Is PHTS always inherited?
No, PTEN gene changes are not always inherited from a parent. They can occur for the first time in a child.
I have a PTEN alteration. What is the chance that I have passed it onto my children?
PHTS is an autosomal dominant genetic condition. This means that if you have a PTEN gene change, there is a 50:50 or 1 in 2 chance of passing this onto children.
- http://www.geneticalliance.org.uk/information/learn-about-genetics/inheritance-patterns/#autosomaldominant
- https://www.genomicseducation.hee.nhs.uk/modes-of-inheritance/autosomal-dominant-inheritance
- https://www.youtube.com/watch?v=oE9BUuv2pTo&list=PLpMgTX_sXoj6kA9i-04a126NP7zGSY-hA&index=2
Can testing be done to predict whether an unborn baby is affected?
It is possible to do a test in pregnancy to find out if a fetus has inherited a PTEN alteration from their mother or father. If the fetus is found to have the PTEN alteration, it is not currently possible to predict how the child will be affected in the future.
- https://www.nhs.uk/conditions/amniocentesis/
- https://www.nhs.uk/conditions/chorionic-villus-sampling-cvs/
Pre-implantation genetic diagnosis is another possible option.
- https://www.hfea.gov.uk/treatments/embryo-testing-and-treatments-for-disease/pre-implantation-genetic-diagnosis-pgd/
- http://www.geneticalliance.org.uk/information/services-and-testing/preimplantation-genetic-diagnosis-information-for-patients/
Genetic Counsellors can talk through options in detail. You can ask your GP or another doctor involved in your care to refer you to your closest Regional Clinical Genetics Service.
Someone else in my family has told me they have PHTS. How do I get a test?
Ask your GP or another doctor involved in your care to refer you to your closest Regional Clinical Genetics Service.
- http://www.bsgm.org.uk/information-education/genetics-centres/
- http://www.bsgm.org.uk/information-education/for-patients/what-happens-at-a-medical-genetics-appointment/
- http://www.geneticalliance.org.uk/information/services-and-testing/nhs-genetic-services-in-the-uk/
- http://www.rarechromo.org/information/Other/A%20Clinical%20Genetics%20Appointment%20FTNW.pdf
Author: Dr Katherine Lachlan, Lead Consultant in Clinical Genetics,
Wessex Clinical Genetics Service, Princess Anne Hospital, Southampton
References
Arch, E. M., Goodman, B. K., Van Wesep, R. A., Liaw, D., Clarke, K., Parsons, R., McKusick, V. A., Geraghty, M. T. Deletion of PTEN in a patient with Bannayan-Riley-Ruvalcaba syndrome suggests allelism with Cowden disease. Am. J. Med. Genet. 71: 489-493, 1997. [PubMed: 9286463, related citations] [Full Text])
Goffin A, Hoefsloot LH, Bosgoed E, Swillen A, Fryns JP. PTEN mutation in a family with Cowden syndrome and autism. Am J Med Genet. 2001;105:521–4.
Butler MG, Dasouki MJ, Zhou XP, Talebizadeh Z, Brown M, Takahashi TN, Miles JH, Wang CH, Stratton R, Pilarski R, Eng C. Subset of individuals with autism spectrum disorders and extreme macrocephaly associated with germline PTEN tumour suppressor gene mutations. J Med Genet. 2005;42:318–21. [PMC free article] [PubMed]
Herman GE, Butter E, Enrile B, Pastore M, Prior TW, Sommer A. Increasing knowledge of PTEN germline mutations: Two additional patients with autism and macrocephaly. Am J Med Genet A. 2007a;143A:589–93. [PubMed]
Herman GE, Henninger N, Ratliff-Schaub K, Pastore M, Fitzgerald S, McBride KL. Genetic testing in autism: how much is enough? Genet Med. 2007b;9:268–74. [PubMed]
Liaw, D., Marsh, D. J., Li, J., Dahia, P. L. M., Wang, S. I., Zheng, Z., Bose, S., Call, K. M., Tsou, H. C., Peacocke, M., Eng, C., Parsons, R. Germline mutations of the PTEN gene in Cowden disease, an inherited breast and thyroid cancer syndrome. Nature Genet. 16: 64-67, 1997. [PubMed: 9140396, related citations] [Full Text]
Varga EA, Pastore M, Prior T, Herman GE, McBride KL. The prevalence of PTEN mutations in a clinical pediatric cohort with autism spectrum disorders, developmental delay and macrocephaly. Genet Med. 2009;11:111–7. [PubMed]